The 21st-century Keller
family. Craig and Sandy are seated at center, with their
daughters Kristy Harden, left, and Rachel. In the rear from left
are Kim Werk, Craig’s sister; Dennis, his brother; and Priscilla
Keller Reynolds, his mother.
ARE WE GOING TO BE
BIGGER, SMARTER AND HEALTHIER THAN
OUR ANCESTORS
The New York Times: July 30, 2006: By GINA KOLATA
Valentin Keller enlisted in an all-German
unit of the Union Army in Hamilton, Ohio, in 1862. He was 26, a small,
slender man, 5 feet 4 inches tall, who had just become a naturalized
citizen. He listed his occupation as tailor.
A year later, Keller was honorably discharged, sick and broken. He had a
lung ailment and was so crippled from arthritis in his hips that he could
barely walk.
His pension record tells of his suffering. “His rheumatism is so that he is
unable to walk without the aid of crutches and then only with great pain,”
it says. His lungs and his joints never got better, and Keller never worked
again.
He died at age 41 of “dropsy,” which probably meant that he had congestive
heart failure, a condition not associated with his time in the Army. His
39-year-old wife, Otilia, died a month before him of what her death
certificate said was “exhaustion.”
People of Valentin Keller’s era, like those before and after them, expected
to develop chronic diseases by their 40’s or 50’s. Keller’s descendants had
lung problems, they had heart problems, they had liver problems. They died
in their 50’s or 60’s.
Now, though, life has changed. The family’s baby boomers are reaching middle
age and beyond and are doing fine.
“I feel good,” says Keller’s great-great-great-grandson Craig Keller. At 45,
Mr. Keller says he has no health problems, nor does his 45-year-old wife,
Sandy.
The Keller family illustrates what may prove to be one of the most striking
shifts in human existence — a change from small, relatively weak and sickly
people to humans who are so big and robust that their ancestors seem almost
unrecognizable.
New research from around the world has begun to reveal a picture of humans
today that is so different from what it was in the past that scientists say
they are startled. Over the past 100 years, says one researcher, Robert W.
Fogel of the University of Chicago, humans in the industrialized world have
undergone “a form of evolution that is unique not only to humankind, but
unique among the 7,000 or so generations of humans who have ever inhabited
the earth.”
And if good health and nutrition early in life are major factors in
determining health in middle and old age, that bodes well for middle-aged
people today. Investigators predict that they may live longer and with less
pain and misery than any previous generation.
“Will
old age for today’s baby boomers be anything like the old age we think we
know?” Dr. Barker asked. “The answer is no.”
Trying to Change a Pattern
Craig Keller does not know what to expect of his old age. But he is
optimistic by nature, and he knows he has already lived past the life span
of his beleaguered ancestor Valentin. He is 5-foot-9, 200 pounds and
exuberantly healthy.
He grew up in Hamilton, the same town on the Kentucky border where Valentin
lived, worshiped and was buried. And he still lives there, working as a
court bailiff, married to Sandy, whom he met when they were in second grade.
Now, married 25 years, the Kellers have two grown daughters, a lively black
dog and no complaints.
Craig and Sandy Keller had all the advantages of middle-class Americans of
their age: childhood vaccines, plenty of food, antibiotics when they fell
ill. Now, wanting to stay healthy, they walk in the evenings, try to eat
well and rely on their strong faith, which, they say, makes a big difference
to their health. And they enjoy life.
Mr. Keller pulls his wife’s tan Chevy Malibu into the driveway of his small,
immaculate house on a sidewalk-lined street. It is the same house that he
grew up in; he and Mrs. Keller bought it from Mr. Keller’s parents 22 years
ago. While Mrs. Keller brings out a snack of a homemade cheese ball,
crackers, sandwiches, fruit salad and brownies, Mr. Keller settles in to
marvel at the contrast between his comfortable life and the lives of his
ancestors.
For him, the idea of falling ill in his late 20’s and never working again is
unimaginable. He knows, though, that he is nearing the age when many of his
ancestors died. His father, Carl D. Keller, a lifelong smoker, developed
prostate cancer, then emphysema, and then lung cancer, which killed him at
age 65. His father’s father, Carl W. Keller, also a smoker, died of cancer
of the esophagus just after he turned 69. His grandfather on his mother’s
side died of cirrhosis of the liver at 55; his grandmother died at 56 of
breast cancer.
“They never got out of their 50’s and 60’s,” Mr. Keller said. “So that’s
kind of in the back of your mind.” He worries about his lungs, given his
family history. He had pneumonia once and has had bronchitis.
But, Mr. Keller reasons, he is so physically different from his ancestors —
he has never smoked and is so much healthier, so much better fed — that he
really thinks he will break the spell.
And if exercise is good for health, the Kellers certainly have exercised.
Mr. Keller displays a bookcase in their basement, crammed with athletic
trophies. Mrs. Keller’s are from baton twirling, Mr. Keller’s are from
baseball, basketball, softball and soccer. Their daughters, 19-year-old
Rachel and 22-year-old Kristy, got theirs cheerleading.
Mrs. Keller said that when she was her daughters’ age, “I didn’t think about
my health very much.”
“But later in my 30’s and toward my 40’s,” she said, “I started to think
about it. You try to eat right, you try to exercise. And you do see your
parents with illnesses. And you wonder about yourself. My mom had a
quadruple bypass when she was 75, and she had to have a pacemaker after
that. She’s now in her 80’s, but you do wonder.”
Was it genetic destiny or health habits that caused her mother’s heart
disease? Mrs. Keller asks herself. Her mother smoked for more than a decade,
finally quitting with great difficulty before Mrs. Keller was born. “She
said the Lord helped her,” Mrs. Keller said.
Mrs. Keller has never smoked. Concerned about heart disease, she had her
cholesterol level tested a few years ago and now takes medication to lower
it. She walks at lunch with the women in her office and after dinner with
her husband.
Her daughter Rachel, petite and quiet with a quick smile, is already
thinking about her family’s medical history. She worries about heart
disease, worries about lung disease. She has already had her cholesterol
level measured — it was normal. And she is shocked when people her age start
smoking.
“In high school, none of my friends smoked,” she said. “They came back from
their first year in college, and all of them did.”
“It’s hard to think about getting old when you’re young,” Rachel added. “But
when you see your family members — my grandpa died of lung cancer, my
grandparents on both sides had cancer. So it’s on my mind a lot of times.”
But still, the future is so distant it is almost unfathomable to her. “I
wonder what we’re going to be like when we’re old,” she mused.
Lives Plagued by Illness
Scientists used to say that the reason people are living so long these days
is that medicine is keeping them alive, though debilitated. But studies like
one Dr. Fogel directs, of Union Army veterans, have led many to rethink that
notion.
The study involves a random sample of about 50,000 Union Army veterans. Dr.
Fogel compared those men, the first generation to reach age 65 in the 20th
century, with people born more recently.
The researchers focused on common diseases that are diagnosed in pretty much
the same way now as they were in the last century. So they looked at
ailments like arthritis, back pain and various kinds of heart disease that
can be detected by listening to the heart.
The
first surprise was just how sick people were, and for how long.
Instead of inferring health from causes of death on death certificates, Dr.
Fogel and his colleagues looked at health throughout life. They used the
daily military history of each regiment in which each veteran served, which
showed who was sick and for how long; census manuscripts; public health
records; pension records; doctors’ certificates showing the results of
periodic examinations of the pensioners; and death certificates.
They discovered that almost everyone of the Civil War generation was plagued
by life-sapping illnesses, suffering for decades. And these were not some
unusual subset of American men — 65 percent of the male population ages 18
to 25 signed up to serve in the Union Army. “They presumably thought they
were fit enough to serve,” Dr. Fogel said.
Even teenagers were ill. Eighty percent of the male population ages 16 to 19
tried to sign up for the Union Army in 1861, but one out of six was rejected
because he was deemed disabled.
And the Union Army was not very picky. “Incontinence of urine alone is not
grounds for dismissal,” said Dora Costa, an M.I.T. economist who works with
Dr. Fogel, quoting from the regulations. A man who was blind in his right
eye was disqualified from serving because that was his musket eye. But, Dr.
Costa said, “blindness in the left eye was O.K.”
After the war ended, as the veterans entered middle age, they were rarely
spared chronic ailments.
“In the pension records there were descriptions of hernias as big as
grapefruits,” Dr. Costa said. “They were held in by a truss. These guys were
continuing to work although they clearly were in a lot of pain. They just
had to cope.”
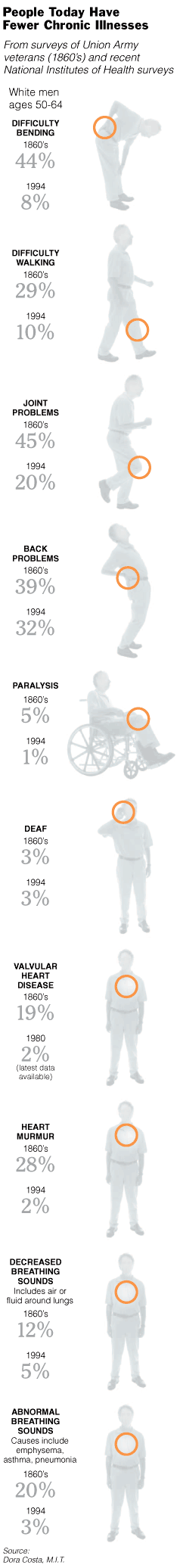
Eighty percent had heart disease by the time they were 60, compared with
less than 50 percent today. By ages 65 to 74, 55 percent of the Union Army
veterans had back problems. The comparable figure today is 35 percent.
The steadily improving health of recent generations shows up in population
after population and country after country. But these findings raise a
fundamental question, Dr. Costa said.
“The question is, O.K., there are these differences, and yes, they are big.
But why?” she said.
“That’s the million-dollar question,” said David M. Cutler, a health
economist at Harvard. “Maybe it’s the trillion-dollar question. And there is
not a received answer that everybody agrees with.”
Outgrowing the Past
Don Hotchkiss, a civil engineer in Las Vegas and a descendant of Civil War
veterans, is an avid Civil War re-enactor. Early on, he and his brother
tried to sleep in an exact replica of one of the old tents.
It was too small, Mr. Hotchkiss said. He is six feet tall and stocky. His
brother, a police officer in Phoenix, is thinner, but 6-foot-2. The tents
were made for men who were average size then. “In the past 145 years, we’ve
ballooned up,” Mr. Hotchkiss said. At a recent meeting of a Las Vegas chapter of the Sons of Confederate
Veterans, eight burly men crowded into a library meeting room. All had
experienced the equivalent of the Civil War tent problem.
“At the re-enactments, all the directors, all the costume directors say the
re-enactors are just too darn big,” said George McClendon, a hefty
67-year-old retired airline pilot.
|
Mr. McClendon is right. Men living in the Civil War era had an average
height of 5-foot-7 and weighed an average of 147 pounds. That translates
into a body mass index of 23, well within the range deemed “normal.” Today,
men average 5-foot-9½ and weigh an average of 191 pounds, giving them an
average body mass index of 28.2, overweight and edging toward obesity.
Those changes, along with the great improvements in general health and life
expectancy in recent years, intrigued Dr. Costa. Common chronic diseases —
respiratory problems, valvular heart disease, arteriosclerosis, and joint
and back problems — have been declining by about 0.7 percent a year since
the turn of the 20th century. And when they do occur, they emerge at older
ages and are less severe.
The reasons, she and others are finding, seem to have a lot to do with
conditions early in life. Poor nutrition in early years is associated with
short stature and lifelong ill health, and until recently, food was
expensive in the United States and Europe.
Dr. Fogel and Dr. Costa looked at data on height and body mass index among
Union Army veterans who were 65 and older in 1910 and veterans of World War
II who were that age in the 1980’s. Their data relating size to health led
them to a prediction: the World War II veterans should have had 35 percent
less chronic disease than the Union Army veterans. That, they said, is
exactly what happened.
They
also found that diseases early in life left people predisposed to chronic
illnesses when they grew older.
“Suppose you were a survivor of typhoid or tuberculosis,” Dr. Fogel said.
“What would that do to aging?” It turned out, he said, that the number of
chronic illnesses at age 50 was much higher in that group. “Something is
being undermined,” he said. “Even the cancer rates were higher. Ye gods. We
never would have suspected that.”
Men who had respiratory infections or measles tended to develop chronic lung
disease decades later. Malaria often led to arthritis. Men who survived
rheumatic fever later developed diseased heart valves.
And stressful occupations added to the burden on the body.
People would work until they died or were so disabled that they could not
continue, Dr. Fogel said. “In 1890, nearly everyone died on the job, and if
they lived long enough not to die on the job, the average age of retirement
was 85,” he said. Now the average age is 62.
A century ago, most people were farmers, laborers or artisans who were
exposed constantly to dust and fumes, Dr. Costa said. “I think there is just
this long-term scarring.”
Searching for Answers
Dr. Barker of Oregon Health and Science University is intrigued by the
puzzle of who gets what illness, and when.
“Why do some people get heart disease and strokes and others don’t?” he
said. “It’s very clear that current ideas about adult lifestyles go only a
small way toward explaining this. You can say that it’s genes if you want to
cease thinking about it. Or you can say, When do people become vulnerable
during development? Once you have that thought, it opens up a whole new
world.”
It is a world that obsesses Dr. Barker. Animal studies and data that he and
others have been gathering have convinced him that health in middle age can
be determined in fetal life and in the first two years after birth.
His work has been controversial. Some say that other factors, like poverty,
may really be responsible. But Dr. Barker has also won over many scientists.
In one study, he examined health records of 8,760 people born in Helsinki
from 1933 to 1944. Those whose birth weight was below about six and a half
pounds and who were thin for the first two years of life, with a body mass
index of 17 or less, had more heart disease as adults.

Another study, of 15,000 Swedish men and women born from 1915 to 1929, found
the same thing. So did a study of babies born to women who were pregnant
during the Dutch famine, known as the Hunger Winter, in World War II.
That famine lasted from November 1944 until May 1945. Women were eating as
little as 400 to 800 calories a day, and a sixth of their babies died before
birth or shortly afterward. But those who survived seemed fine, says Tessa
J. Roseboom, an epidemiologist at the University of Amsterdam, who studied
2,254 people born at one Dutch hospital before, during and after the famine.
Even their birth weights were normal.
But now those babies are reaching late middle age, and they are starting to
get chronic diseases at a much higher rate than normal, Dr. Roseboom is
finding. Their heart disease rate is almost triple that of people born
before or after the famine. They have more diabetes. They have more kidney
disease.
That is no surprise, Dr. Barker says. Much of the body is complete before
birth, he explains, so a baby born to a pregnant woman who is starved or ill
may start life with a predisposition to diseases that do not emerge until
middle age.
The middle-aged people born during the famine also say they just do not feel
well. Twice as many rated their health as poor, 10 percent compared with 5
percent of those born before or after the famine.
“We asked them whether they felt healthy,” Dr. Roseboom said. “The answer to
that tends to be highly predictive of future mortality.”
But not everyone was convinced by what has come to be known as the Barker
hypothesis, the idea that events very early in life affect health and
well-being in middle and old age. One who looked askance was Douglas V.
Almond, an economist at Columbia University.
Dr. Almond had a problem with the studies. They were not of randomly
selected populations, he said, making it hard to know if other factors had
contributed to the health effects. He wanted to see a rigorous test — a
sickness or a deprivation that affected everyone, rich and poor, educated
and not, and then went away. Then he realized there had been such an event:
the 1918 flu.
The flu pandemic arrived in the United States in October 1918 and was gone
by January 1919, afflicting a third of the pregnant women in the United
States. What happened to their children? Dr. Almond asked.
He compared two populations: those whose mothers were pregnant during the
flu epidemic and those whose mothers were pregnant shortly before or shortly
after the epidemic.
To his astonishment, Dr. Almond found that the children of women who were
pregnant during the influenza epidemic had more illness, especially
diabetes, for which the incidence was 20 percent higher by age 61. They also
got less education — they were 15 percent less likely to graduate from high
school. The men’s incomes were 5 percent to 7 percent lower, and the
families were more likely to receive welfare.
The effects, Dr. Almond said, occurred in whites and nonwhites, in rich and
poor, in men and women. He convinced himself, he said, that there was
something to the Barker hypothesis.
Craig Keller hopes it is true. He looks back at the hard life of his
ancestors, even those of his great-grandfather and his grandfather, working
as painters, exposed to fumes. And, of course, there was poor Valentin
Keller, his Civil War ancestor, his health ruined by the time he was 30.
Today, Mr. Keller says, he is big and healthy, almost despite himself. He
would like to think it is because he tries to live well, but he is not so
sure, especially when he hears about what Dr. Barker and Dr. Fogel and the
others have found. Maybe it was his good fortune to have been born to a
healthy mother and to be well fed and vaccinated.
“I don’t know if we have as much control as we think we do,” he said.
The difference does not involve changes in genes, as far as is known, but
changes in the human form. It shows up in several ways, from those that are
well known and almost taken for granted, like greater heights and longer
lives, to ones that are emerging only from comparisons of health records.
The biggest surprise emerging from the new studies is that many chronic
ailments like heart disease, lung disease and arthritis are occurring an
average of 10 to 25 years later than they used to. There is also less
disability among older people today, according to a federal study that
directly measures it. And that is not just because medical treatments like
cataract surgery keep people functioning. Human bodies are simply not
breaking down the way they did before.
Even the human mind seems improved. The average I.Q. has been increasing for
decades, and at least one study found that a person’s chances of having
dementia in old age appeared to have fallen in recent years.
The proposed reasons are as unexpected as the changes themselves. Improved
medical care is only part of the explanation; studies suggest that the
effects seem to have been set in motion by events early in life, even in the
womb, that show up in middle and old age.
“What happens before the age of 2 has a permanent, lasting effect on your
health, and that includes aging,” said Dr. David and J. P. Barker, a professor
of medicine at Oregon Health and Science University in Portland and a
professor of epidemiology at the University of Southampton in England.
Each event can touch off others. Less cardiovascular disease, for example,
can mean less dementia in old age. The reason is that cardiovascular disease
can precipitate mini-strokes, which can cause dementia. Cardiovascular
disease is also a suspected risk factor for Alzheimer’s disease.
The effects are not just in the United States. Large and careful studies
from Finland, Britain, France, Sweden and the Netherlands all confirm that
the same things have happened there; they are also beginning to show up in
the underdeveloped world.
Of course, there were people in previous generations who lived long and
healthy lives, and there are people today whose lives are cut short by
disease or who suffer for years with chronic ailments. But on average, the
changes, researchers say, are huge.
Even more obvious differences surprise scientists by the extent of the
change.
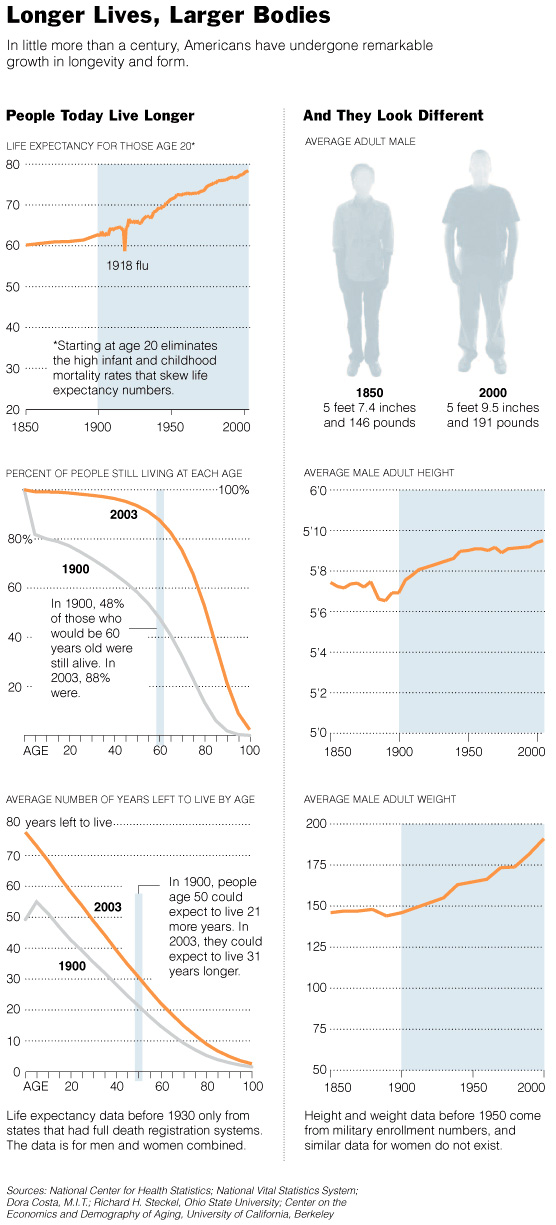
In 1900, 13 percent of people who were 65 could expect to see 85. Now,
nearly half of 65-year-olds can expect to live that long.
People even look different today. American men, for example, are nearly
three inches taller than they were 100 years ago and about 50 pounds
heavier.
“We’ve been transformed,” Dr. Fogel said.
What next? scientists ask.
Today’s middle-aged people are the first
generation to grow up with childhood vaccines and with antibiotics. Early
life for them was much better than it was for their parents, whose early
life, in turn, was much better than it was for their parents.
(This is the first article in a series looking at the science of aging. Other
articles will explore the genetics of aging, body image and frailty, and who
ages well and why.)
Below are comparative
charts showing the changes occurring in human body and health..... |